Innovative Firsts: 90 Years of Partnering for Patients


Massachusetts is a state of bold firsts.
Home to the nation’s first public school, the first subway system, and even the basketball game, the commonwealth has long been a place where new ideas take shape and endure.
Nowhere is that legacy more prominent than healthcare. From lifesaving clinical advancements adopted around the world to innovative models of care delivery that touch every local neighborhood, Massachusetts hospitals and health systems have always led the way.
For 90 years, the Massachusetts Health & Hospital Association has stood alongside our member organizations as they advance a legacy of innovation, driven by a shared commitment to improving patient lives, empowering caregivers, and strengthening communities.
Below are examples of innovative “firsts” and forward‑thinking innovations
from local hospitals and health systems over the years.

 Developed at Baystate Health, the G.E.M.M.E. (Global Emergency Medicine Metric Evaluation) tool is an innovative solution to emergency department congestion, enabling near real-time, systemwide decision-making to improve operations and reduce overcrowding. Now implemented across all five emergency departments and the Women’s Evaluation and Treatment Unit, G.E.M.M.E. provides a unified framework that integrates data visibility, multidisciplinary coordination, and proactive escalation, and is accessible to teams through both a web-based platform and a mobile application.
Developed at Baystate Health, the G.E.M.M.E. (Global Emergency Medicine Metric Evaluation) tool is an innovative solution to emergency department congestion, enabling near real-time, systemwide decision-making to improve operations and reduce overcrowding. Now implemented across all five emergency departments and the Women’s Evaluation and Treatment Unit, G.E.M.M.E. provides a unified framework that integrates data visibility, multidisciplinary coordination, and proactive escalation, and is accessible to teams through both a web-based platform and a mobile application.
Rather than relying on retrospective analysis or siloed interventions, the tool aligns frontline teams, hospital leadership, and support services around shared metrics that drive action. It translates complex operational pressures into clear, structured steps that can be deployed across sites, standardizing how bottlenecks are identified, resources are mobilized, and progress is monitored.
This implementation has shifted ED throughput from a reactive challenge to a coordinated system priority. It strengthens collaboration, improves situational awareness, and enhances the ability to respond to changing patient volumes and acuity. As health systems face persistent capacity constraints, G.E.M.M.E. offers a scalable, replicable approach to modernizing operations and delivering timely, high-quality, patient-centered care.
The Greenfield Family Medicine Residency at UMass Chan Medical School – Baystate is the only family medicine training program serving Western Massachusetts. Created to address the needs of rural communities, the program is redefining physician training to improve access to care in underserved areas. Located at Baystate Franklin Medical Center, the residency places trainees in the community and prepares them to provide comprehensive, relationship-based care where it is most needed.
The residency features a modern curriculum focused on outpatient primary care, physician wellbeing, and adaptability to changing patient needs. Its small cohort model encourages close mentorship, flexibility, and meaningful clinical experiences, while enabling residents to help shape the program and influence the region’s healthcare landscape.
 The program stands out for its ability to retain physicians in the communities it serves, achieving a 75% retention rate since its first graduating class in 2024. This is a key benchmark in addressing rural workforce shortages. By aligning training with community needs, Baystate Health is building a sustainable pipeline of highly skilled family physicians who understand the populations they serve.
The program stands out for its ability to retain physicians in the communities it serves, achieving a 75% retention rate since its first graduating class in 2024. This is a key benchmark in addressing rural workforce shortages. By aligning training with community needs, Baystate Health is building a sustainable pipeline of highly skilled family physicians who understand the populations they serve.
As health systems nationwide face increasing access challenges, the Greenfield Family Medicine Residency provides a model for community-based training that strengthens local care, supports physician resilience, and promotes long-term health equity in Western Massachusetts.

Berkshire Health Systems (BHS) has long been a leader in rural healthcare in the commonwealth, relying on innovative care models and careful planning to maintain access to quality care across the region. As home to two of Massachusetts’ four Critical Access Hospitals (CAHs), and the commonwealth’s only system to operate more than one CAH, BHS has demonstrated how alternative care models can not only maintain, but also strengthen access to care across rural communities. For the system, the critical access model is a core element of the organization’s long-term strategic plan and an essential tool for bringing the BHS mission to life.
 Fairview Hospital consistently ranks among the nation’s top CAHs 13 years running. In fact, it was recently honored among the Top 20 Critical Access Hospitals in America by The Chartis Center and the National Rural Health Association. Recognizing the success of this model at Fairview Hospital, BHS leadership worked for many years in collaboration with its Congressional delegation to identify and support changes to the federal CAH requirements, opening a path for BHS to reopen North Adams Regional Hospital, which had operated as a satellite facility under Berkshire Medical Center’s license for a decade after closing under its previous ownership. In 2024, this goal became a reality, and BHS successfully reopened North Adams Regional Hospital as a fully licensed Critical Access Hospital.
Fairview Hospital consistently ranks among the nation’s top CAHs 13 years running. In fact, it was recently honored among the Top 20 Critical Access Hospitals in America by The Chartis Center and the National Rural Health Association. Recognizing the success of this model at Fairview Hospital, BHS leadership worked for many years in collaboration with its Congressional delegation to identify and support changes to the federal CAH requirements, opening a path for BHS to reopen North Adams Regional Hospital, which had operated as a satellite facility under Berkshire Medical Center’s license for a decade after closing under its previous ownership. In 2024, this goal became a reality, and BHS successfully reopened North Adams Regional Hospital as a fully licensed Critical Access Hospital.
Today, both North Adams Regional Hospital and Fairview Hospital play a crucial role in BHS’ operating model. Leveraging the organization’s flagship community teaching hospital, Pittsfield’s Berkshire Medical Center, alongside CAHs in northern and southern Berkshire County, BHS delivers essential local services while seamlessly connecting patients to higher levels of care when needed. Coupled with a robust outpatient network, clinics, pharmacies, and home care, this model keeps care coordinated, accessible, and community based.
By building a system that links award-winning expertise with community-based care, BHS continues to set the standard for how CAHs can sustain rural health for generations.
Recruitment has always been particularly challenging in rural areas, worsened by the impact of COVID-19 on the national healthcare workforce shortage. In 2021, Berkshire Health Systems (BHS), like peers nationwide, relied heavily on travel clinicians and other short-term solutions to support its workforce and provide continued access to care. While these solutions addressed an immediate need, BHS needed to be forward-thinking in exploring innovative paths to meaningfully bolster its workforce in the long term. BHS decided to develop a pipeline of skilled clinicians in Berkshire County called the Career Pathways Program.
 Through BHS’s Career Pathways Program, the system offers paid, structured training opportunities that open doors to in-demand clinical roles. Career Pathways combines in-house training, full-time pay and benefits, and academic partnerships with local educational leaders like Berkshire Community College and McCann Technical School. In fact, in 2023, BHS collaborated with Massachusetts College of Liberal Arts (MCLA) to launch a new four-year Bachelor of Science in Nursing Program with a paid, Pathways component for eligible students. This growing “earn while you learn” model has become a leading example of how a health system can use local investment to transform both careers and care delivery in its community.
Through BHS’s Career Pathways Program, the system offers paid, structured training opportunities that open doors to in-demand clinical roles. Career Pathways combines in-house training, full-time pay and benefits, and academic partnerships with local educational leaders like Berkshire Community College and McCann Technical School. In fact, in 2023, BHS collaborated with Massachusetts College of Liberal Arts (MCLA) to launch a new four-year Bachelor of Science in Nursing Program with a paid, Pathways component for eligible students. This growing “earn while you learn” model has become a leading example of how a health system can use local investment to transform both careers and care delivery in its community.
Within Career Pathways, BHS currently offers multiple paid training tracks, each tied to clear roles and advancement opportunities:
- Nursing Assistant: Acute care training in direct patient care, that can bridge to long-term nursing careers.
- Medical Assistant: Full-time paid program with classroom and hands-on practice experiences.
- Licensed Practical Nurse (LPN): Work-and-learn progression from entry-level to LPN roles.
- Associate Degree in Nursing (ADN): Support through ADN into registered nursing positions, easing rural barriers.
- Bachelor of Science in Nursing (BSN): New four-year program with MCLA for local BSN pipeline.
- Respiratory Therapist: Targeted placements for hard-to-fill rural specialty roles.
- Sonography: Training in high-demand imaging positions.
- Biomedical Engineering: In-house talent for clinical equipment support.
As of October 1, 2025, the Pathways Program has produced measurable, system-wide impact:
- 250 graduates of the Modified Nursing Assistant Program with 178 currently employed
- 139 graduates of the Medical Assistant program, with 87 currently employed
- 53 graduates of the Associate Degree in Nursing program, with 52 currently employed and 127 currently enrolled
- 47 graduates of the Licensed Practical Nurse program, with 34 currently employed
- 12 students currently enrolled in the Respiratory Therapist Program
- 2 students enrolled in the Sonography program
Unlike health systems that rely primarily on external pipelines, BHS has deliberately built a comprehensive internal pathway structure that supports workforce development for hundreds of local residents per year and allows the organization to take a step toward revitalizing the region through the creation of new jobs. Thanks to its unique model of coupling high-level training with paid employment and benefits, the BHS Pathways Program also reduces barriers to access for community members who were previously unable to join the field due to economic or logistical challenges. Together with the funding provided through MassHire grants and the organization’s education partners, this long-term, locally anchored investment has positioned BHS as a statewide leader in healthcare workforce development and as a model for how rural systems can create their own sustained talent pipelines.

 Monica Wojcik, M.D., MPH, is a leader in advancing precision genomic medicine at Boston Children’s Hospital, where she serves as Medical Director of the Manton Center Gene Discovery Core, Attending Physician in the Divisions of Newborn Medicine and Genetics and Genomics, and Assistant Director of Robert’s Program on Sudden Unexpected Death in Pediatrics. Her work focuses on improving diagnostic speed and accuracy for critically ill newborns, where time-sensitive decisions can significantly alter outcomes.
Monica Wojcik, M.D., MPH, is a leader in advancing precision genomic medicine at Boston Children’s Hospital, where she serves as Medical Director of the Manton Center Gene Discovery Core, Attending Physician in the Divisions of Newborn Medicine and Genetics and Genomics, and Assistant Director of Robert’s Program on Sudden Unexpected Death in Pediatrics. Her work focuses on improving diagnostic speed and accuracy for critically ill newborns, where time-sensitive decisions can significantly alter outcomes.
Dr. Wojcik played a key role in a groundbreaking collaboration between Boston Children’s Hospital, Broad Clinical Labs, and Roche Sequencing Solutions that achieved the fastest human whole genome sequencing to date. The team developed and piloted a same-day sequencing workflow designed specifically for neonatal intensive care unit (NICU) patients, where traditional genetic testing can take days. In testing 15 samples, including seven from NICU patients, the method reduced the time from sample receipt to genetic data in about four hours, with the fastest full turnaround from sample to report completed in just 6 hours and 47 minutes.
 This achievement, recognized by GUINNESS WORLD RECORDS™, represents a major step toward making rapid genomic diagnosis feasible in routine clinical care. As first author of the peer-reviewed study published in the New England Journal of Medicine, Dr. Wojcik emphasized the potential impact on critically ill infants, noting that same-day results could transform decision-making in the NICU by enabling earlier, more targeted interventions.
This achievement, recognized by GUINNESS WORLD RECORDS™, represents a major step toward making rapid genomic diagnosis feasible in routine clinical care. As first author of the peer-reviewed study published in the New England Journal of Medicine, Dr. Wojcik emphasized the potential impact on critically ill infants, noting that same-day results could transform decision-making in the NICU by enabling earlier, more targeted interventions.
Her work continues to advance the integration of genomic sequencing into point-of-care settings, with the goal of shortening diagnostic timelines and improving outcomes for infants with suspected rare or genetic conditions.

In 1910, the Flexner Report set forth the structure and processes of U.S. medical education. In the century that followed, medicine’s approach to clinical education changed very little.
 Meanwhile, the fields of education, neurobiology, and social and cognitive psychology advanced greatly, propelling our understanding of how people learn. In 2004, Harvard Medical School and Cambridge Health Alliance aimed to further students’ scientific and clinical learning, sense of duty, and humanistic care. The result was a breakthrough innovation — the first academic longitudinal integrated clerkship. This program, the Harvard Medical School Cambridge Integrated Clerkship (HMS-CIC), redesigned the core clinical training in medical school by translating the principles of the empirical sciences of learning into a new educational structure.
Meanwhile, the fields of education, neurobiology, and social and cognitive psychology advanced greatly, propelling our understanding of how people learn. In 2004, Harvard Medical School and Cambridge Health Alliance aimed to further students’ scientific and clinical learning, sense of duty, and humanistic care. The result was a breakthrough innovation — the first academic longitudinal integrated clerkship. This program, the Harvard Medical School Cambridge Integrated Clerkship (HMS-CIC), redesigned the core clinical training in medical school by translating the principles of the empirical sciences of learning into a new educational structure.
This rigorous approach to learning and caregiving ensures and advances students’ knowledge and skills and their commitment to patients. The new model creates meaningful and authentic roles for students. Rather than serving as brief, peripheral participants on inpatient teams, HMS-CIC students assume heightened roles through apprenticeship under experienced faculty. In the HMS-CIC, students and their faculty specialists together care for a panel of patients over the course of one year, with the highest standards, accountability, and extended engagement with their patients. The HMS-CIC has demonstrated highly successful outcomes for learning and retention, patient care, and transferability across specialties, institutions, and contexts. After multiple academic studies produced strong outcome data, the innovation achieved wide reach, furthering clinical education transformation nationwide (now more than 30% of U.S. schools) and worldwide (nearly half the schools in Canada and Australia among many other nations). The HMS-CIC is now driving innovations across the continuum of medical education and advancing the discourse in health professions education more generally.
 The Victims of Violence (VOV) Program at Cambridge Health Alliance (CHA) is widely regarded as a foundational pillar of modern trauma-informed care. Founded in 1984 with start-up funds from the City of Cambridge as a training program of Harvard Medical School’s Department of Psychiatry at Cambridge Hospital, it developed comprehensive mental health services for crime victims and crime-victimized communities.
The Victims of Violence (VOV) Program at Cambridge Health Alliance (CHA) is widely regarded as a foundational pillar of modern trauma-informed care. Founded in 1984 with start-up funds from the City of Cambridge as a training program of Harvard Medical School’s Department of Psychiatry at Cambridge Hospital, it developed comprehensive mental health services for crime victims and crime-victimized communities.
VOV popularized a structured, three-phase approach to trauma recovery that is now standard practice:
- Safety and Stabilization: Prioritizing the patient’s physical and emotional safety before delving into trauma.
- Remembrance and Mourning: Processing the trauma in a controlled, therapeutic environment.
- Reconnection: Helping the survivor re-enter the community and build a future.
The program received numerous honors, including the Innovations Award from the Massachusetts Office for Victim Assistance (MOVA), which cited its creative community partnerships and effective treatment models. In 1988, it received the American Psychiatry Association’s Gold Award for innovative hospital and community service.
VOV helped make trauma-informed care central to mental health treatment at organizations across the country. With practitioners better equipped to treat trauma victims, the program was integrated into clinical operations at CHA in 2022. Its legacy continues to shape the global mental health field.

Long before urgent care became a standard part of the healthcare landscape, Emerson identified a critical access gap: patients relied on the emergency department for non-emergent conditions, driving up costs, increasing wait times, and straining hospital capacity. Emerson acted early, adopting urgent care as a deliberate strategy to redesign access and create a more appropriate, convenient, and cost-effective entry point into the healthcare system.
 Over the past decade, Emerson expanded this vision by opening three urgent care locations across the region and supporting more than 48,000 patient visits annually. These sites ensure patients can access care where and when they need it. Building on this foundation, Emerson introduced virtual urgent care to further remove barriers and launched Emerson Health Connected Care — an innovative, concierge-light model that partners with local employers to proactively guide employees to the right care at the right time. Together, these efforts reflect a forward-thinking approach that improves patient experience, reduces unnecessary emergency department utilization, and strengthens community health.
Over the past decade, Emerson expanded this vision by opening three urgent care locations across the region and supporting more than 48,000 patient visits annually. These sites ensure patients can access care where and when they need it. Building on this foundation, Emerson introduced virtual urgent care to further remove barriers and launched Emerson Health Connected Care — an innovative, concierge-light model that partners with local employers to proactively guide employees to the right care at the right time. Together, these efforts reflect a forward-thinking approach that improves patient experience, reduces unnecessary emergency department utilization, and strengthens community health.
As demand for digestive health services grew, particularly for endoscopy and colorectal cancer screening, Emerson recognized an opportunity to fundamentally rethink care delivery. Providers traditionally delivered these services in hospital settings, where they often cost more and offered less convenience for patients.
 In 2022, Emerson opened a dedicated outpatient Digestive Health and Endoscopy Center, intentionally shifting care to a more accessible, patient-centered, and cost-efficient model. Emerson designed this facility to meet patients where they are, offering streamlined scheduling, a comfortable setting, and high-quality care outside of the hospital environment.
In 2022, Emerson opened a dedicated outpatient Digestive Health and Endoscopy Center, intentionally shifting care to a more accessible, patient-centered, and cost-efficient model. Emerson designed this facility to meet patients where they are, offering streamlined scheduling, a comfortable setting, and high-quality care outside of the hospital environment.
The Digestive Health Center expands access to essential screenings, including colonoscopies that support early cancer detection, and aligns with a broader industry shift toward ambulatory care. Emerson continues to lead in this space by proactively adapting care delivery models to improve outcomes, lower costs, and better meet growing patient demand.

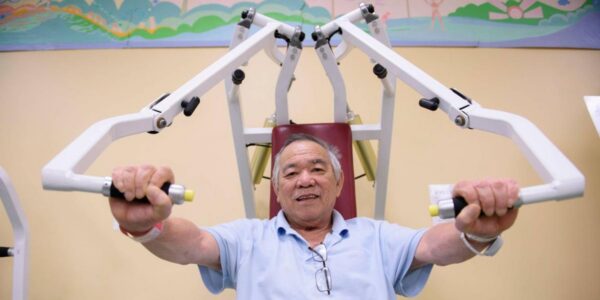 In the 1990s, it was widely believed that strength training was dangerous for older people. While some research existed on strength training in healthy people in their 60s and 70s, there were almost no studies on significantly older adults with frailty in long-term care settings. Hebrew SeniorLife’s research institute aimed to test that widespread belief through two studies led by Dr. Maria Fiatarone Singh. The studies explored the effects of strength training on long-term care residents in their 80s and 90s. The study results did more than challenge beliefs — they affected how people view aging and strength. According to a pilot study, over just eight weeks of training, nine residents aged 87 to 96 showed an average strength increase of 174%. Researchers didn’t observe the cardiovascular problems that doctors feared. A follow-up study in the New England Journal of Medicine in 1994 saw tremendous gains in those doing progressive resistance training, including a 113% average increase in leg strength, improved walking speed, stair climbing ability, and spontaneous physical activity.
In the 1990s, it was widely believed that strength training was dangerous for older people. While some research existed on strength training in healthy people in their 60s and 70s, there were almost no studies on significantly older adults with frailty in long-term care settings. Hebrew SeniorLife’s research institute aimed to test that widespread belief through two studies led by Dr. Maria Fiatarone Singh. The studies explored the effects of strength training on long-term care residents in their 80s and 90s. The study results did more than challenge beliefs — they affected how people view aging and strength. According to a pilot study, over just eight weeks of training, nine residents aged 87 to 96 showed an average strength increase of 174%. Researchers didn’t observe the cardiovascular problems that doctors feared. A follow-up study in the New England Journal of Medicine in 1994 saw tremendous gains in those doing progressive resistance training, including a 113% average increase in leg strength, improved walking speed, stair climbing ability, and spontaneous physical activity.
 Hebrew SeniorLife has established the Lunder CareForce Institute, supported by a generous commitment from the Lunder Foundation, to address the growing shortage of frontline health care workers by offering comprehensive training and career advancement in health and aging-related programs. The Institute also provides support for individuals who face language, technology, or financial obstacles to pursuing education. It builds on the success of the nursing assistant training program, which was established in 2021 to help employees seeking to change their career paths and others attain their certifications.
Hebrew SeniorLife has established the Lunder CareForce Institute, supported by a generous commitment from the Lunder Foundation, to address the growing shortage of frontline health care workers by offering comprehensive training and career advancement in health and aging-related programs. The Institute also provides support for individuals who face language, technology, or financial obstacles to pursuing education. It builds on the success of the nursing assistant training program, which was established in 2021 to help employees seeking to change their career paths and others attain their certifications.
The Institute provides opportunities for nursing assistant training and other programs designed to advance career opportunities for frontline staff. It aims to reduce barriers by providing financial support, English language and computer training, and academic and life coaching.
Hebrew SeniorLife is offering nursing assistant training and is partnering with other skilled nursing facilities to train more student groups. It is also partnering with employers to guarantee job placement after students successfully complete training and certification.
Hebrew SeniorLife plans to start a licensed practical nurse training program and, ideally, programs for more advanced nursing degrees, creating even more career pathways for interested individuals. Over the next 10 years, Hebrew SeniorLife estimates it can reach more than 3,000 students in Massachusetts alone, including current employees, through a variety of training programs. This project is funded by the Senator Kenneth J. Donnelly Workforce Success Grant (Workforce Competitiveness Trust Fund FY’24-25 Appropriation). This grant initiative is administered by Commonwealth Corporation on behalf of the Executive Office of Labor and Workforce Development and the Workforce Skills Cabinet.

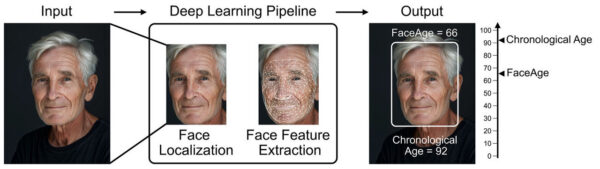 FaceAge is an innovative artificial intelligence–driven tool developed by Mass General Brigham researchers that leverages simple photos of a person’s face to estimate a biological age, which could be reflective of their overall health status. By integrating deep learning with clinical data, FaceAge has demonstrated the ability to predict important health outcomes, including survival rates and treatment tolerance for people with cancer. This type of information provides clinicians with an additional, non-invasive data point to guide decision-making, personalize treatment plans, and improve risk stratification. Prior to a tool like FaceAge, this type of decision-making, such as how aggressive of a treatment plan to prescribe a patient with cancer, could include many subjective factors, such as an “eyeball test.” In several studies published within the last several months, the team has shown that people who had an older FaceAge compared to their chronological age had poorer outcomes following cancer treatment. The team is currently planning prospective clinical trials that leverage FaceAge, to further test its viability as a tool with clinical application. The research team has also launched an online research portal that allows the public to submit their own face photos to get a FaceAge assessment, and help advance the tool, at faceage.bwh.harvard.edu.
FaceAge is an innovative artificial intelligence–driven tool developed by Mass General Brigham researchers that leverages simple photos of a person’s face to estimate a biological age, which could be reflective of their overall health status. By integrating deep learning with clinical data, FaceAge has demonstrated the ability to predict important health outcomes, including survival rates and treatment tolerance for people with cancer. This type of information provides clinicians with an additional, non-invasive data point to guide decision-making, personalize treatment plans, and improve risk stratification. Prior to a tool like FaceAge, this type of decision-making, such as how aggressive of a treatment plan to prescribe a patient with cancer, could include many subjective factors, such as an “eyeball test.” In several studies published within the last several months, the team has shown that people who had an older FaceAge compared to their chronological age had poorer outcomes following cancer treatment. The team is currently planning prospective clinical trials that leverage FaceAge, to further test its viability as a tool with clinical application. The research team has also launched an online research portal that allows the public to submit their own face photos to get a FaceAge assessment, and help advance the tool, at faceage.bwh.harvard.edu.
What makes FaceAge a true “innovative first” is its use of everyday imaging — standard patient photographs, such as those taken during routine visits to the clinic — as a powerful diagnostic signal. It transforms a simple, low-cost input into actionable clinical intelligence, expanding the role of AI in medicine. As healthcare continues to move toward precision medicine, FaceAge represents a breakthrough in how we assess aging and can personalize care with a better understanding of a patient’s overall health. By making biological age measurable in a scalable and accessible way, it has the potential to enhance clinical judgment, improve patient outcomes and redefine how health systems evaluate risk across diverse populations.
Mass General Brigham’s Mobile Postpartum Care Unit (MPCU) redefines how postpartum care is delivered by bringing comprehensive, hospital-level services directly to patients in their communities.
 Using Mass General Brigham’s Community Care Vans, the team delivers multidisciplinary care curbside at postpartum individual’s homes, including physical exams, lactation support, mental health screening, blood pressure management, and coordinated follow-up planning for patients at high risk of postpartum complications. Clinicians also provide up to six free follow-up visits, along with direct connections to mental health care, housing resources, medically tailored meals and financial supports for a year postpartum.
Using Mass General Brigham’s Community Care Vans, the team delivers multidisciplinary care curbside at postpartum individual’s homes, including physical exams, lactation support, mental health screening, blood pressure management, and coordinated follow-up planning for patients at high risk of postpartum complications. Clinicians also provide up to six free follow-up visits, along with direct connections to mental health care, housing resources, medically tailored meals and financial supports for a year postpartum.
Traditional postpartum care can be disjointed, and for patients facing physical, social, or structural barriers such as transportation challenges, childcare needs, and scheduling constraints, follow-up is often difficult or inaccessible. The MPCU closes these gaps by bringing care directly into neighborhoods and even into patients’ homes, enabling earlier identification of complications, including hypertensive disorders, mood concerns, and feeding difficulties.
This model shifts postpartum care from episodic, reactive visits to proactive, relationship-based ones that are delivered in real-world environments, while also advancing equity by reducing barriers that disproportionately affect underserved patients. In its first 20 months, the program enrolled 135 high-risk individuals, more than half experiencing housing or food insecurity and greater than two-thirds needing mental health or behavior support. All participants received hypertension care, and 100% of them avoided emergency department visits or hospital readmissions while enrolled.
By embedding advanced postpartum care within a mobile, community-based model, the MPCU demonstrates how health systems can redesign care delivery to better support vulnerable patients and their families.

 Merrimack Health has invested in the da Vinci robotic surgery platform, brining this advanced robotic-assisted surgery program to the communities in the Merrimack Valley through Methuen Hospital. This investment reflects Merrimack Health’s broader, system-wide planning for care delivery, as it continuously assesses where to expand services, where consolidation can improve quality and efficiency, and where new capabilities are beneficial to meeting the needs of patients and providers. Importantly, it expands access to this advanced surgical option within the Merrimack Valley, helping ensure patients can receive care in their community.
Merrimack Health has invested in the da Vinci robotic surgery platform, brining this advanced robotic-assisted surgery program to the communities in the Merrimack Valley through Methuen Hospital. This investment reflects Merrimack Health’s broader, system-wide planning for care delivery, as it continuously assesses where to expand services, where consolidation can improve quality and efficiency, and where new capabilities are beneficial to meeting the needs of patients and providers. Importantly, it expands access to this advanced surgical option within the Merrimack Valley, helping ensure patients can receive care in their community.
 In partnership with Top Notch Scholars, a Lawrence-based youth leadership nonprofit, Merrimack Health is hosting a series of healthcare panel presentations designed to introduce high school students to the wide range of career opportunities in the field. Supported by the Atrius Health Equity Foundation grant, these panels bring together Merrimack Health professionals from both clinical and non-clinical roles to share real-world insights, personal experiences, and practical guidance. To date, more than 90 students from the city of Lawrence have attended. Through this collaboration, students gain early exposure to careers they may not have previously considered, helping to broaden their perspective and open pathways into health care. At the same time, the initiative strengthens efforts to build a more connected, inspired, and locally rooted pipeline of future healthcare talent for our community.
In partnership with Top Notch Scholars, a Lawrence-based youth leadership nonprofit, Merrimack Health is hosting a series of healthcare panel presentations designed to introduce high school students to the wide range of career opportunities in the field. Supported by the Atrius Health Equity Foundation grant, these panels bring together Merrimack Health professionals from both clinical and non-clinical roles to share real-world insights, personal experiences, and practical guidance. To date, more than 90 students from the city of Lawrence have attended. Through this collaboration, students gain early exposure to careers they may not have previously considered, helping to broaden their perspective and open pathways into health care. At the same time, the initiative strengthens efforts to build a more connected, inspired, and locally rooted pipeline of future healthcare talent for our community.

Patients in the greater Taunton area now have access to a new, incisionless weight-loss option.
Morton Hospital expanded its weight loss capabilities in the spring of 2026 and is the region’s first program specializing in minimally invasive endobariatric procedures, designed to help patients achieve meaningful, long-lasting weight loss without incisions or hospital stays.
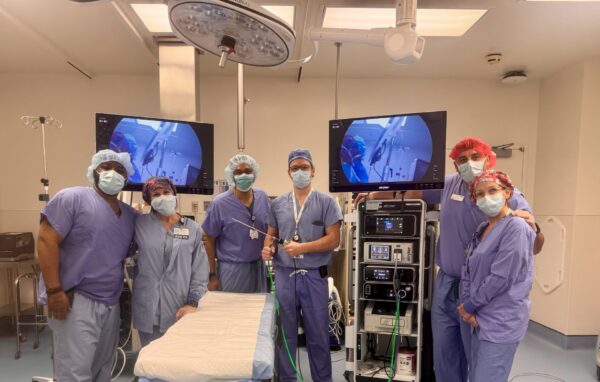 David Leenen, MD, a member of the Brown Health Medical Group surgical team at Morton Hospital, is currently the only surgeon in the area to perform ESG (endoscopic sleeve gastroplasty) and TORe (transoral outlet reduction) procedures. ESG and TORe offer patients a non-surgical pathway to meaningful, sustained weight loss by reshaping the stomach from the inside using advanced endoscopic techniques, reducing stomach volume to promote portion control and supporting weight loss in patients with obesity and related metabolic conditions.
David Leenen, MD, a member of the Brown Health Medical Group surgical team at Morton Hospital, is currently the only surgeon in the area to perform ESG (endoscopic sleeve gastroplasty) and TORe (transoral outlet reduction) procedures. ESG and TORe offer patients a non-surgical pathway to meaningful, sustained weight loss by reshaping the stomach from the inside using advanced endoscopic techniques, reducing stomach volume to promote portion control and supporting weight loss in patients with obesity and related metabolic conditions.
Morton Hospital is a Surgical Quality Partner of the American College of Surgeons (ACS) and is accredited as a low-acuity center by the Metabolic and Bariatric Surgery Accreditation and Quality Improvement Program (MBSAQIP), certified by the ACS and the American Society for Metabolic and Bariatric Surgery. MBSAQIP accreditation reflects adherence to rigorous national standards for safety, quality, and outcomes in bariatric care.
In 2023, Morton Hospital began offering upper airway stimulation therapy, “Inspire,” a breakthrough obstructive sleep apnea treatment option for those who cannot use or tolerate Continuous Positive Airway Pressure (CPAP) therapy.
 Morton Hospital was the first in the region – and is currently the only hospital in Southeastern Massachusetts – to offer this treatment option, which involves an FDA-approved implantable device that prevents airway obstruction during sleep. Inspire works inside the body with a patient’s natural breathing process to treat sleep apnea. Mild stimulation opens the airway during sleep, allowing oxygen to flow naturally. The patient uses a small handheld remote to turn the device on before bed and off when they wake up. The program is led by Ameer Shah, MD, otolaryngology specialist and director of the hospital’s Inspire Upper Airway Stimulation Therapy Program, as well as Imad Bahhady, MD, pulmonary critical care and sleep medicine specialist, who serves as the medical director of the hospital’s Center for Sleep Medicine.
Morton Hospital was the first in the region – and is currently the only hospital in Southeastern Massachusetts – to offer this treatment option, which involves an FDA-approved implantable device that prevents airway obstruction during sleep. Inspire works inside the body with a patient’s natural breathing process to treat sleep apnea. Mild stimulation opens the airway during sleep, allowing oxygen to flow naturally. The patient uses a small handheld remote to turn the device on before bed and off when they wake up. The program is led by Ameer Shah, MD, otolaryngology specialist and director of the hospital’s Inspire Upper Airway Stimulation Therapy Program, as well as Imad Bahhady, MD, pulmonary critical care and sleep medicine specialist, who serves as the medical director of the hospital’s Center for Sleep Medicine.
“In our practice we see many patients who have stopped using or are unable to tolerate CPAP,” said Dr. Bahhady. “Inspire represents a significant advancement in treating sleep apnea. It is clinically proven to reduce sleep apnea events, has a high level of patient satisfaction and a high therapy adherence. We are excited and fortunate to offer this promising therapy to sleep apnea patients who struggle with CPAP.”
This spring, Morton Hospital is scheduled to perform its 100th Inspire implant.

Saint Anne’s Hospital has become the first hospital in southeastern Massachusetts to perform renal denervation, marking a significant innovation in the treatment of uncontrolled hypertension. The groundbreaking procedure was led by interventional cardiologist Sadip Pant, MD, offering new hope to patients whose blood pressure remains dangerously elevated despite maximum medical therapy.
Renal denervation is a minimally invasive therapy that targets overactive nerves surrounding the renal arteries – key contributors to persistent high blood pressure. For patients at high risk of stroke, heart failure, and cardiovascular death, treatment options have traditionally been limited. By introducing this advanced therapy locally, Saint Anne’s is expanding access to cutting-edge cardiovascular care for the region.
 The procedure was performed by Dr. Pant in collaboration with vascular surgeon Ibrahim Eid, MD, and supported by a highly skilled, multidisciplinary team spanning cardiology, vascular surgery, nursing, and the cardiac catheterization laboratory. Their collaboration underscores the hospital’s commitment to clinical excellence and innovation. “This milestone reflects the extraordinary teamwork and expertise of our cardiovascular specialists,” said Carole Billington, RN, MSN, NEA-BC, president and chief nursing officer. “Most importantly, it represents a meaningful step forward for patients facing life-threatening hypertension.”
The procedure was performed by Dr. Pant in collaboration with vascular surgeon Ibrahim Eid, MD, and supported by a highly skilled, multidisciplinary team spanning cardiology, vascular surgery, nursing, and the cardiac catheterization laboratory. Their collaboration underscores the hospital’s commitment to clinical excellence and innovation. “This milestone reflects the extraordinary teamwork and expertise of our cardiovascular specialists,” said Carole Billington, RN, MSN, NEA-BC, president and chief nursing officer. “Most importantly, it represents a meaningful step forward for patients facing life-threatening hypertension.”
This achievement reinforces Saint Anne’s mission to bring advanced, high-quality care to the community — ensuring patients receive the latest treatments close to home.
Saint Anne’s Hospital, a member of Brown University Health, has launched an innovative partnership with the Somerset Fire Department to improve survival outcomes for patients experiencing sepsis – a life-threatening medical emergency – before they arrive at the hospital. This first-of-its-kind collaboration in Bristol County enables Somerset EMS to administer IV antibiotics in the field, allowing life-saving treatment to begin minutes earlier than traditional emergency care.
 Grounded in emerging research showing significantly reduced mortality with early antibiotic intervention, the program focuses on rapid identification and treatment of sepsis at first EMS contact. Paramedics screen patients upon arrival, and those meeting clinical criteria receive immediate antibiotics, accelerating care during the most critical window of illness.
Grounded in emerging research showing significantly reduced mortality with early antibiotic intervention, the program focuses on rapid identification and treatment of sepsis at first EMS contact. Paramedics screen patients upon arrival, and those meeting clinical criteria receive immediate antibiotics, accelerating care during the most critical window of illness.
The initiative was spearheaded by Saint Anne’s emergency services leaders Ian Dennen, MSN, R.N., and Andrew Old, M.D., who led comprehensive training for Somerset paramedics. Training included the use of advanced medication infusion pumps, lactate monitoring technology, and enhanced protocols for prehospital antibiotic administration.
“This partnership extends the hospital’s capabilities into the field and gives patients a critical head start in treatment,” said Dennen.
The collaboration reflects a shared commitment between Saint Anne’s Hospital and Somerset Fire and Rescue to innovation, early intervention, and community health. By combining advanced technology, education, and cross-agency teamwork, this program represents a meaningful advancement in emergency care and reinforces Saint Anne’s mission to improve outcomes through forward-thinking, community-based solutions.

A Level II Trauma Center title is the second-highest designation a hospital can earn and indicates that it can accept the most seriously injured patients in a medical emergency. Clinically, it can perform the same services and procedures as a Level I Trauma Center; the only difference involves academic and research requirements.
For decades, Rhode Island offered the closest hospital with advanced trauma care for patients in southeastern Massachusetts. Travel to Providence cost precious time, delaying the start of critical care.
In 2017, Southcoast Health identified the critical need for a trauma center in the South Coast region and embarked upon the journey with a full assessment of resources that would be required, followed by months of planning and internal investment.
 Then, in 2021, St. Luke’s Hospital earned official designation from the Massachusetts Department of Public Health as a Level II Adult Trauma Center – becoming the first and only Level II Trauma Center in the Massachusetts EMS Region 5 serving southeastern Massachusetts.
Then, in 2021, St. Luke’s Hospital earned official designation from the Massachusetts Department of Public Health as a Level II Adult Trauma Center – becoming the first and only Level II Trauma Center in the Massachusetts EMS Region 5 serving southeastern Massachusetts.
Today, the center treats more than 2,000 patients annually.
When COVID-19 struck, Southcoast Health knew that the most effective way to get people tested was to meet them where they were – community centers, local businesses…even fishing boats and piers.
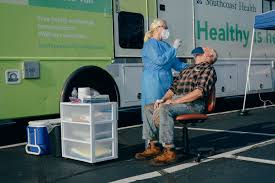 New Bedford is one of the country’s most important fishing centers. Roughly 390 million pounds of seafood a year come through the city. A third of that is fished locally, while the rest comes from other countries and is processed here. With so many employees working in close contact, the docks and processing plants could have become a COVID “superspreader” site, but Southcoast Health partnered with the city’s health department on a testing initiative to turn mobile units normally used as flu clinics into free COVID-19 testing centers that could test processing plant employees and meet ships at the pier. With results available in 24 to 48 hours, Southcoast healthcare workers could vet crew members during the two- to three-day windows they remain on shore between fishing trips. This testing program was so innovative and successful that it was covered by National Geographic magazine.
New Bedford is one of the country’s most important fishing centers. Roughly 390 million pounds of seafood a year come through the city. A third of that is fished locally, while the rest comes from other countries and is processed here. With so many employees working in close contact, the docks and processing plants could have become a COVID “superspreader” site, but Southcoast Health partnered with the city’s health department on a testing initiative to turn mobile units normally used as flu clinics into free COVID-19 testing centers that could test processing plant employees and meet ships at the pier. With results available in 24 to 48 hours, Southcoast healthcare workers could vet crew members during the two- to three-day windows they remain on shore between fishing trips. This testing program was so innovative and successful that it was covered by National Geographic magazine.
When vaccines became available, Southcoast Health adopted a similar approach, meeting people where they were with convenient vaccination clinics across the region. Ultimately, we administered 114,000+ vaccine doses in the first year.

For four decades, Tufts Medical Center has been at the forefront of cardiac innovation and life-saving care. On October 30, 2025, the hospital proudly celebrated the 40th anniversary of its very first heart transplant. Today, Tufts Medical Center is recognized as a national leader and is home to New England’s number one heart transplant program.
The Advanced Heart Failure and Cardiac Transplantation Program has consistently set the standard for clinical excellence. Since 2000, Tufts Medical Center has performed 727 adult heart transplants – the most in New England, outpacing the next-closest center by more than 70 procedures during that time.
 The program’s momentum and dedication to patient outcomes only continue to grow. In 2024, Tufts Medical Center achieved a historic milestone by transplanting more adult hearts than any other center in the region, breaking its own previous record set in 2023. The surgical team performed an astounding 70 heart transplants that year, achieving a remarkable 100% survival rate.
The program’s momentum and dedication to patient outcomes only continue to grow. In 2024, Tufts Medical Center achieved a historic milestone by transplanting more adult hearts than any other center in the region, breaking its own previous record set in 2023. The surgical team performed an astounding 70 heart transplants that year, achieving a remarkable 100% survival rate.
As we celebrate Hospital Week, Tufts Medical Center’s heart transplant program stands as a shining example of dedication, expertise, and the power of advanced medicine to give patients a second chance at life.
When aspiring doctors go through medical school, they learn to diagnose and treat illness – but the human side of medicine is rarely part of the curriculum. Tufts Medicine and Tufts University School of Medicine (TUSM) are changing that with the Medical Interviewing and the Doctor-Patient Relationship (MIDPR) program, an innovative initiative designed to bridge the gap between medical education and compassionate clinical care.
Offered to TUSM first-year medical students each fall, MIDPR combines two components: classroom instruction led by registered nurse educators – who teach students how to talk to patients and understand each person’s unique experience of illness – and hands-on practice conducting real medical interviews with hospitalized and ambulatory patients at Tufts Medicine’s community hospitals, Lowell General Hospital, and MelroseWakefield Hospital.
 Now in its second year, the program has earned rave reviews from nurse educators, medical students, and patients alike. Research has long supported the value of nurses – known for their bedside manner and interpersonal skills – in teaching medical students, and MIDPR puts that principle into action. Students rotate between observer and interviewer roles in small groups, exploring weekly clinical topics such as nutrition, mental health, mobility, oncology, and end-of-life care, while also learning to address patients’ social determinants of health.
Now in its second year, the program has earned rave reviews from nurse educators, medical students, and patients alike. Research has long supported the value of nurses – known for their bedside manner and interpersonal skills – in teaching medical students, and MIDPR puts that principle into action. Students rotate between observer and interviewer roles in small groups, exploring weekly clinical topics such as nutrition, mental health, mobility, oncology, and end-of-life care, while also learning to address patients’ social determinants of health.
To Tufts Medicine’s knowledge, this model has not been replicated anywhere else. By embedding the human element into medical training from day one, MIDPR is producing a new generation of physicians who are not only clinically skilled, but also more empathetic, collaborative, and prepared to earn the trust of the patients they serve.

 UMass Memorial Health launched its virtual idea platform, Innovation Station, in 2012 to encourage caregivers to collaborate and develop actionable solutions to frontline challenges. Since then, the platform has achieved a caregiver participation rate of 95% and supported the implementation of more than 200,000 ideas. Innovation Station empowers frontline teams to identify efficiency gaps, address everyday operational challenges, and surface issues the system might not otherwise detect. Over the past year alone, the platform has implemented more than 15,000 ideas and delivered $50 million in cost savings and revenue generation.
UMass Memorial Health launched its virtual idea platform, Innovation Station, in 2012 to encourage caregivers to collaborate and develop actionable solutions to frontline challenges. Since then, the platform has achieved a caregiver participation rate of 95% and supported the implementation of more than 200,000 ideas. Innovation Station empowers frontline teams to identify efficiency gaps, address everyday operational challenges, and surface issues the system might not otherwise detect. Over the past year alone, the platform has implemented more than 15,000 ideas and delivered $50 million in cost savings and revenue generation.
 UMass Memorial Health continues to lead in home-based care programs, including Hospital at Home, Subacute Rehab at Home, and Mobile Integrated Health. These innovative solutions not only work to address persistent capacity challenges across UMass Memorial Health, but they also advance important health equity efforts by increasing access to timely, high-quality care.
UMass Memorial Health continues to lead in home-based care programs, including Hospital at Home, Subacute Rehab at Home, and Mobile Integrated Health. These innovative solutions not only work to address persistent capacity challenges across UMass Memorial Health, but they also advance important health equity efforts by increasing access to timely, high-quality care.
1. UMMH has a nationally recognized Hospital at Home program, which has seen over 3,000 patients since its launch in 2021. Serving more than 20 cities and towns in central Massachusetts, the program provides patients with high-quality, hospital-grade care in the comfort and familiarity of their own home. The program is equipped with a team of field nurses and the organization’s mobile integrated health paramedics to meet the needs of patients with acute conditions or illnesses with low complication rates, including COVID-19, the flu, urinary tract infections, acute kidney injuries, and other acute conditions. The program offers at-home, hospital-level nursing care twice a day, telemedicine visits, delivery of food and supplies, and transportation for testing.
- UMass Memorial creates digital hospital to centralize care and provide patient assistance throughout Central Mass.
- UMass Memorial readies for remote and AI tech with new ‘digital hospital’
2. Subacute Rehab at Home brings skilled nursing and rehabilitative care to patients’ homes – offering medication delivery, vital monitoring, food and supply delivery, respiratory care, diagnostic testing, transportation assistance, and interpreter services. Through a telehealth-enabled tablet, the program allows patients to receive 24/7 access to their care team. This innovative program allows patients to heal in the comfort of their own homes while also helping to shorten hospital length of stay and facilitate successful discharges.
3. Mobile Integrated Health is an innovative care model that provides on-demand care from highly skilled paramedics using portable diagnostics and remote monitoring capabilities to assess symptoms and share with UMMH experts in real time. The program operates from UMMH’s Digital Hub, a 20,000-square-foot, state-of-the-art space for digital medicine services and virtual care delivery.


 Massachusetts Health & Hospital Association
Massachusetts Health & Hospital Association